A rash is characterized by irritated and/or swollen skin, often accompanied by itchiness, pain, and redness. Certain rashes can even result in blistering or the formation of raw skin patches. Rashes can occur as a symptom of various medical conditions, allergies, or exposure to irritating substances. While some rashes appear suddenly, others may gradually develop over several days. While most rashes tend to resolve swiftly, some may persist and require ongoing treatment. Identifying the underlying cause of the rash is crucial for effective treatment.
Acne
Acne is a common skin condition that occurs when hair follicles in the skin become clogged. This blockage, often caused by excess dead skin cells and sebum (skin oils), creates an environment for bacteria to thrive. As a result, inflammation, redness, pain, and swelling can occur. Acne manifests in various forms, including blackheads (open plugged follicles), cystic acne (deep, painful, pus-filled lesions), nodules (large, solid lesions deep beneath the skin), papules (inflamed lesions that are pink and tender), pimples/pustules (papules with white or yellow pus-filled tops), and whiteheads (plugged follicles that remain beneath the skin and produce white bumps). Acne can affect individuals of all ages and races, but it is most commonly observed in teenagers and young adults. While acne often resolves by the time individuals reach their 30s, some people may continue to experience skin problems.
Treatment for acne typically involves a combination of topical and oral medications. Topical medications are available in various forms such as creams, gels, lotions, pads, and soaps. They may include antibiotics (used in conjunction with other topical medications), benzoyl peroxide (which kills bacteria and reduces sebum production), resorcinol (helps break down blackheads and whiteheads), retinoids (derived from vitamin A, prevent acne formation, reduce inflammation, and minimize scarring), salicylic acid (breaks down blackheads and whiteheads, reduces skin cell shedding), and sulfur (breaks down blackheads and whiteheads). Oral medications are often prescribed alongside topical treatments and can consist of antibiotics (slowing bacterial growth and reducing inflammation), corticosteroids (reserved for severe nodular acne, reduces inflammation, can be injected into affected areas), hormone therapy (primarily for women, reduces the impact of androgens on sebaceous glands), and retinoids (facilitates pore opening, prevents acne formation, and reduces scarring).
Atopic Dermatitis (Eczema)
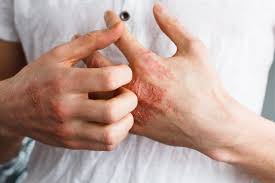
Atopic Dermatitis (Eczema) is a common rash that typically begins in childhood but can occur at any age. Although many individuals with atopic dermatitis see their symptoms resolve during their teenage years, unfortunately, some people continue to experience symptoms throughout adulthood.
This condition causes severe itching of the skin, and scratching only worsens the irritation, leading to cracking, redness, and swelling. In some cases, the affected areas may produce a clear discharge that results in crusting. Atopic dermatitis follows a cycle of remission, during which the skin appears clear, and flares, during which the skin worsens.
The primary treatment goals for atopic dermatitis are to control dry skin, manage itching, prevent flares and infections, promote healing, and reduce inflammation. The treatment approach typically involves a combination of therapies tailored to the specific affected area, patient age, and the severity of the infection. To decrease inflammation and prevent flares, calcineurin inhibitors such as cyclosporine and tacrolimus are commonly used.
Injectable biological medications like dupilumab are employed to block specific functions of the immune response. Moisturizing creams play a crucial role in restoring the skin barrier. Oral Janus kinase inhibitors, including tofacitinib, are reserved for more severe cases and require close monitoring. Steroid creams and ointments are utilized to reduce inflammation. Topical phosphodiesterase-4 inhibitors such as apremilast, crisaborole, and roflumilast are indicated for cases of refractory inflammation.
Rosacea
Rosacea is a chronic, common inflammatory skin condition that typically affects the areas around the cheeks, chin, forehead, and nose. It can also be occasionally seen on the chest, neck, or other areas of the body. It presents with broken blood vessels, pimples, and redness. Rosacea usually occurs after middle age and is more common in individuals with fair skin and women in menopause.
Rosacea has four subtypes:
- erythematotelangiectatic rosacea,
- ocular rosacea,
- papulopustular rosacea, and
- phymatous rosacea.
Erythematotelangiectatic rosacea is characterized by flushing, redness, and visible blood vessels. Ocular rosacea manifests with red eyes, swollen eyelids, and sometimes resembles a stye. Papulopustular rosacea leads to acne-like breakouts, redness, and swelling. Phymatous rosacea causes thickening of the skin and a bumpy texture.
It is important to encourage patients to seek treatment for rosacea as it can spread to the eyes (ocular rosacea) and affect both long- and short-term vision. The treatment goals include improving the patient’s quality of life, preventing complications and worsening of symptoms, and controlling the condition.
In mild cases, topical medications are usually prescribed initially. These may include creams, gels, and ointments containing antibiotics, antiparasitics, or vasoconstrictors to treat flushing and redness. For patients with eye irritation, ophthalmic preparations containing antibiotics, immunosuppressants, and lubricants can be used.
For moderate to severe cases or when ocular involvement is present, oral medications containing antibiotics may be prescribed due to their antibiotic and anti-inflammatory properties. In more severe cases, isotretinoin can be considered as a treatment option.